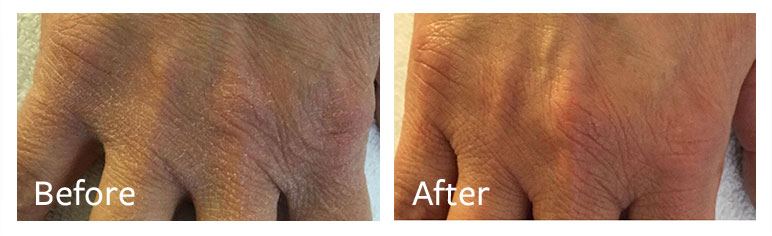
Introducing ReadyMedical
ReadyMedical is the first line of ready-to-mix sterile cosmetic topical products which are specifically formulated to maximize results and improve the appearance of the skin. ReadyMedical’s innovative mixing system guarantees 100% product stability, improved efficacy, and contamination-free cosmetic topical application without added preservatives.
ReadyMedical Cosmetic Products

POST-TREATMENT
Hyaluronic Acid + Perfluorodecalin + Physalis Angulata

How it Works
ReadyMedical features a unique mixing system that allows the practitioner to combine sterile hyaluronic acid with a selected complex of active ingredients, right at the moment of application!

Sterile.
No Preservatives.
The unique mixing system ensures that:
- The ingredients remain stable in the package
- The ingredients are sterile
- No preservatives are added
- The products can be safely applied
HYALURONIC ACID
Hyaluronic acid is the backbone of all ReadyMedical products, as it effectively carries the active cosmetic ingredients that are applied on the skin and protects them from premature degradation.
The result is a 100% pure, chemical-free Hyaluronic acid gel with enhanced aesthetic properties, including improved stability and more effective cosmetic topical.
Anti-Aging Solution
Hyaluronic Acid + Growth Factors
ReadyMedical Anti-Aging Solution maximizes the effect of professional anti-aging treatments. The growth factors are made in a unique process that mimics the activity of native growth factors, with 100% biocompatibility and improved potency and stability.


Skin Healing Solution
Hyaluronic Acid+Perfluorodecalin+Physalis Angulata
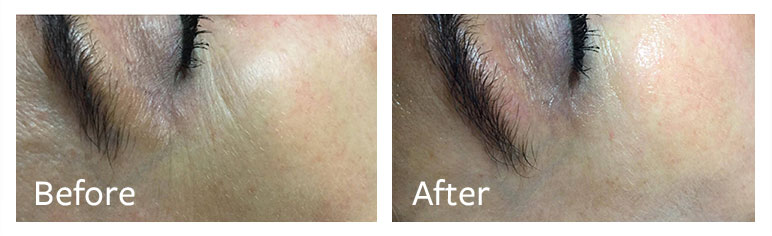
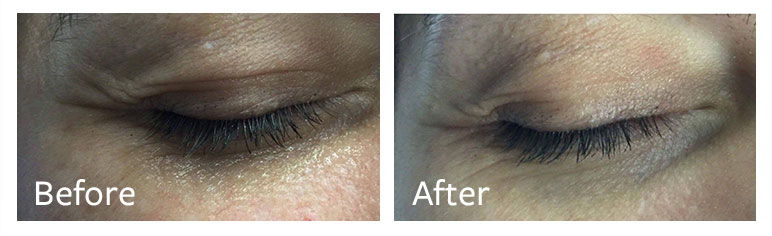
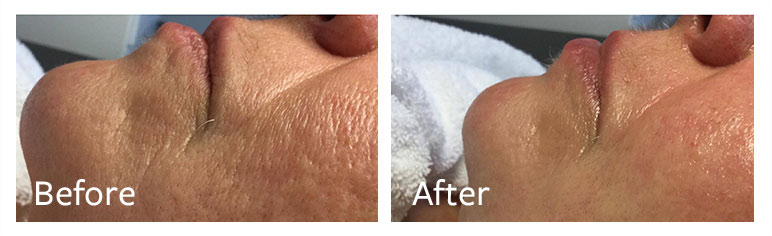
ReadyMedical Skin Healing Solution provides a powerful wound-healing effect after more invasive medical-aesthetic treatments when quick skin repairing is needed.
An independent study[2] by the University of Pavia, Italy, found that inflamed fibroblasts treated with ReadyMedical Skin Healing Solution demonstrated dramatic and significant decrease in the production of pro-inflammatory cytokines when compared to untreated fibroblasts.

Antioxidant Solution
Hyaluronic Acid + Vitamin C


ACNYCID SOLUTION
Hyaluronic Acid + AC Complex
Designed to be used immediately after professional in-clinic treatments that aim to improve the quality of acne-affected skin.
An independent study[4] by the University of Pavia, Italy, found that p. acne bacterial loads were reduced by 99.9% after the bacteria was exposed to ReadyMedical Acne Solution, suggesting long-term inhibition of the bacteria.



REVITALIZING

POST-TREATMENT

ANTIOXIDANT

ACNYCID
Book a Demo
Fill out the form to schedule a personalized demo with our team. We’re excited to connect with you and explore how we can help grow your esthetics business!